

Advanced Strategies in CSF Leak Prevention and Skull Base Reconstruction: Insights from China’s Leading Neurosurgeons
1. Conference Overview
The Chinese Neurosurgical Society (CNS) is the most authoritative and influential academic association for neurosurgeons in China. As part of this year’s CNS Annual Meeting, Medprin hosted a dedicated conference symposium focused on Cerebrospinal Fluid (CSF) Leak Prevention and Management, underscoring its commitment to advancing neurosurgical outcomes through material innovation and clinical collaboration.
The event gathered a total of 18 neurosurgeons from 15 hospitals, with speakers representing top-tier neurosurgical centers across China
The symposium was opened by the session chair, who emphasized that prevention is the cornerstone of managing iatrogenic CSF leaks. The session was structured to comprehensively address the full spectrum of CSF leak management—from prevention to treatment to outcome evaluation—featuring six keynote presentations, six case discussions, and six expert ommentaries.
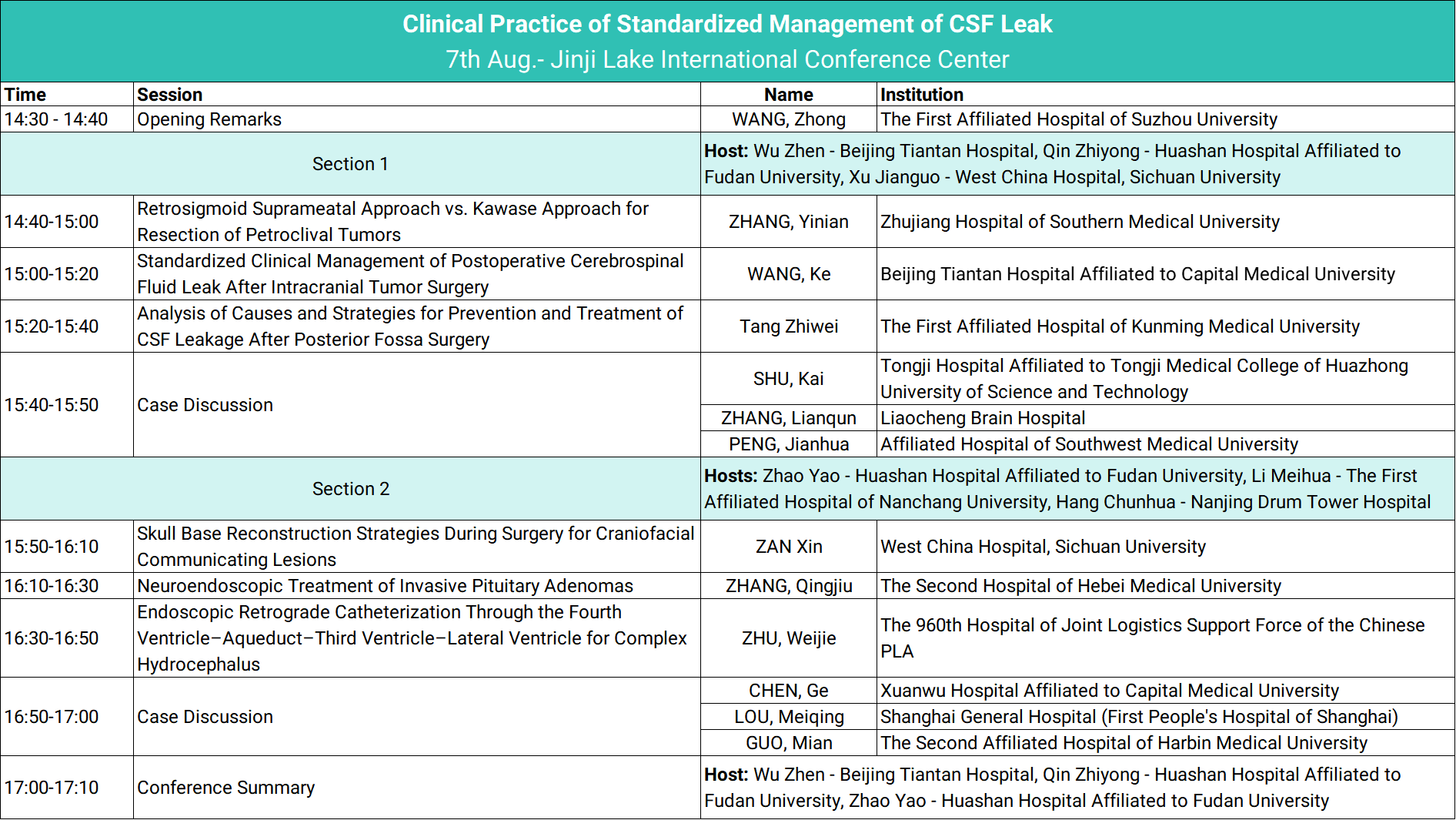

The symposium was divided into two focused sessions:
The first half highlighted CSF management under neurosurgical microscopy
The second half emphasized neuroendoscopic applications and challenges
2.Session I: Microscope-Assisted CSF Management
Post-tumor resection CSF leak management is just as technically demanding as the tumor resection itself, requiring detailed anatomical knowledge and precise surgical skills.
Retrosigmoid Intradural Suprameatal Approach vs. Kawase Approach for Resection of Petroclival Tumors
ZHANG, Yinian – Zhujiang Hospital of Southern Medical University
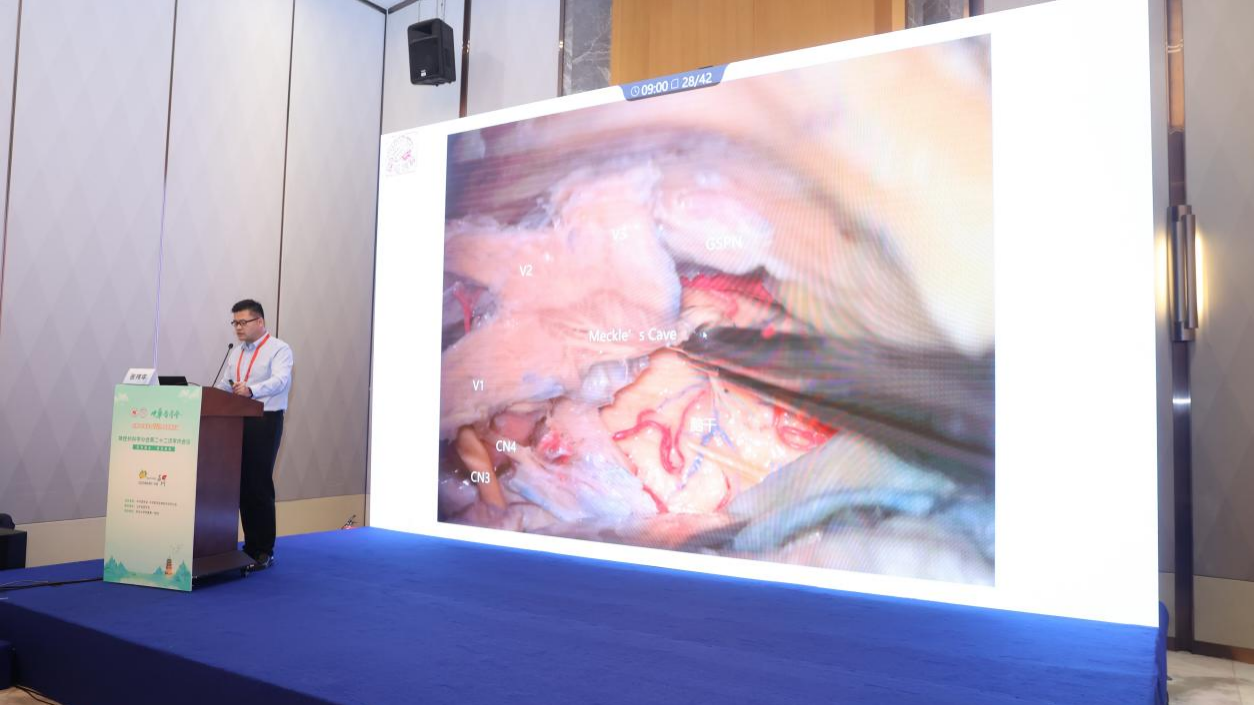
Petroclival tumors are technically demanding due to their proximity to critical cranial nerves. Dr. Zhang presented two surgical approaches: the retrosigmoid intradural suprameatal approach (RSMA), recommended by Professor Samii and sometimes referred to as a “reverse Kawase,” and the standard Kawase approach.
Key technical considerations:
RSMA: Emphasis on preservation of the petrosal vein and facial nerve.
Kawase: Key risks include Labbe vein injury, temporal lobe contusion, and facial nerve damage.
In tight surgical spaces, smaller venous branches may be sacrificed. The two approaches offer different exposure fields.
RSMA highlights: Simpler craniotomy, efficient exposure, extended visualization with extreme lateral supracerebellar infratentorial (SCIT) view; ideal for ipsilateral lesions.
Kawase highlights: Early devascularization of tumor, extended exposure with Dolenc or posterior petrosal variants.
Shared principle: CSF leak prevention must be integrated into surgical planning.
Q&A insight: In vestibular schwannoma cases, preserving the petrosal vein is recommended. If sacrifice is unavoidable, coagulation should be performed close to the dural base to preserve venous drainage and reduce postoperative edema.
——————————————————————————————————————————————
Standardized Clinical Management of Postoperative CSF Leak After Intracranial Tumor Surgery
WANG, Ke – Beijing Tiantan Hospital
Dr. Wang emphasized that the core principle in preventing cerebrospinal fluid (CSF) leakage after craniotomy is restoring the integrity of both the dura and skull base anatomy.
Strategies to ensure watertight closure:
Use non-absorbable monofilament sutures
Combine dural suturing with sealants
Core principle: Anatomical reconstruction of dura and skull base is essential to prevent CSF leak.
Key measures:
Seal bony defects and dural breaches
Postoperative management includes intracranial pressure reduction, cough suppression, and possible lumbar drainage if persistent leakage is suspected
Case series:
Dr. Wang presented six different repair strategies, including:
RSMA with petrous bone reconstruction
Subtemporal approaches
Jugular foramen skull base reconstruction
Recurrence-based anterior skull base repairs
Clinoidectomy-related defects
Tissue reconstruction methods:
Fat grafts
Artificial dura (with or without sutures)
Fascial grafts
Vascularized myocutaneous flaps
Imaging-guided planning:
Use high-resolution CT and MR cisternography to localize bone thinning or leaks
Plan repair material and flap harvesting accordingly
Commentary: Fascial closure is critical where possible. Sutures should match the gauge of the needle to avoid CSF oozing. Hidden bone defects, especially at the petrous apex (Kawase triangle), require meticulous sealing.
——————————————————————————————————————————————
Analysis of Causes and Strategies for Prevention and Treatment of CSF Leakage After Posterior Fossa Surgery
Tang Zhiwei – The First Affiliated Hospital of Kunming Medical University
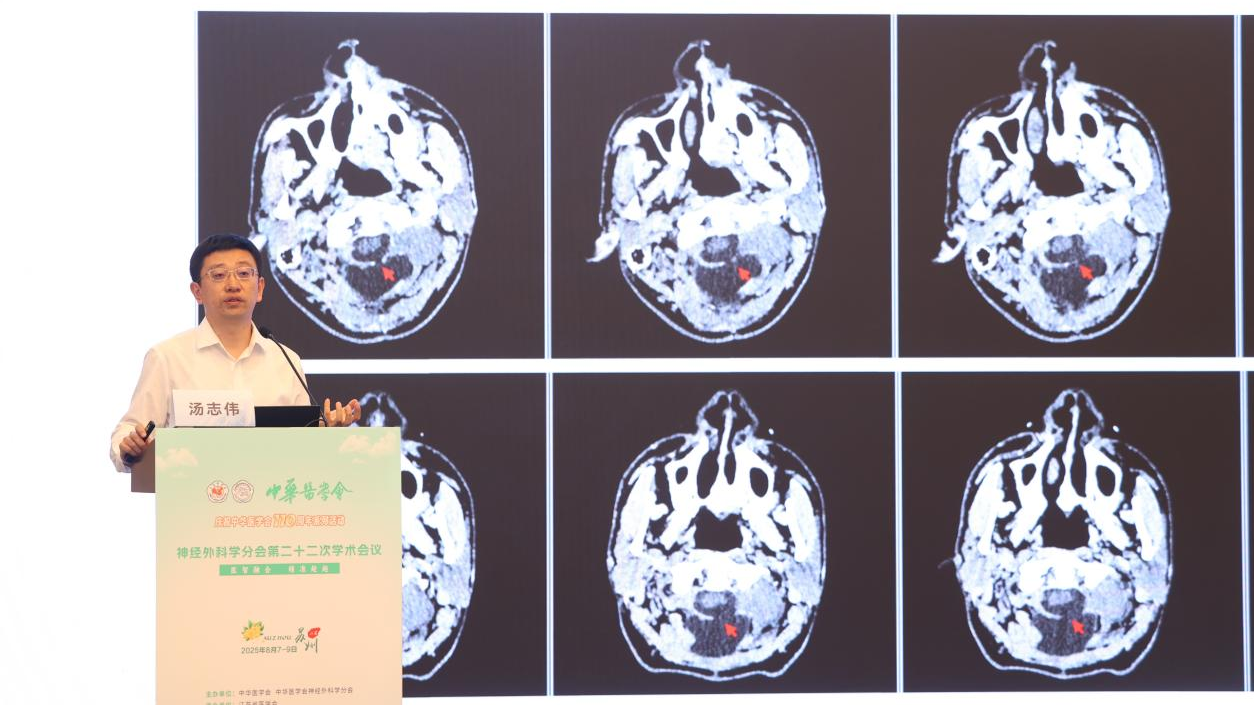
Dr. Tang emphasized that posterior fossa craniotomies carry the highest incidence of postoperative CSF leakage, with sub-tentorial approaches having reported rates as high as 32%.
Leakage can typically originate from:
Dural defects
Bony defects, especially when the bone is aerated or communication exists with mastoid air cells or sinuses.
Case Studies: Six Revision Surgeries for CSF Leak
Leak caused by bony defect exacerbated by post-COVID coughing: Repaired with fat graft + dural sealant
Leak from artificial dura resorption: Repaired with fascia lata + bio-glue
Leak at transverse sinus suture line: Repaired with fascia lata
Needle hole leaks prevented with glue post-suturing
Small defect after IAC drilling: Managed conservatively with bed rest
Combined dural-bony defect + air cell exposure: Repaired with multilayer technique using fat, fascia, bone dust, and sealants
Additional methods:
Bone cement preferred over autologous bone in certain cases due to resorption issues
Summary:
Dura: Watertight, low-tension suturing; reinforce with artificial or autologous grafts
Bone: Bone wax, autologous tissue, or synthetic substitutes for air cell sealing
Soft tissue: Eliminate dead space, layered closure of muscles with crossing techniques
Future directions: Development of synthetic replacements for fascia and fat to reduce donor site morbidity.
——————————————————————————————————————————————
3.Session II: Endoscopic CSF Leak Management
Skull Base Reconstruction Strategies During Surgery for Craniofacial Communicating Lesions
ZAN Xin – West China Hospital, Sichuan University

Core Concept: “Soft–Hard Combined” Reconstruction
1.Soft Tissue Reconstruction:
The key principle is to create a physical barrier between the subdural space and the nasal cavity. Dr. Zan advocated for a hierarchy of preferred materials:
Vascularized regional fascia or muscle flaps (e.g., pedicled temporalis fascia or muscle)
Free vascularized fascial (or myocutaneous) grafts
Free autologous tissue
Synthetic materials (as last resort)
Fixation methods include suturing, press-fit placement, or rigid support.
2.Hard Tissue Reconstruction:
The goal is to cover osseous defects and resist CSF pulsation. Preferred materials:
Original bone flap (if preserved)
Local autologous bone
Resorbable synthetic material
Non-resorbable prosthetics
Fixation options: screws, snap-fit insertion, or supportive structural framing.
Technical Tips Shared:
Simulate CSF pulsation to test watertightness of repair intraoperatively.
For large defects requiring multiple dural graft patches, non-resorbable sutures should be used between patches to ensure watertight closure.
The defect edge often heals rapidly, and resorbable materials may be used peripherally.
Conclusion Summary:
Preoperative Planning: Thin-slice CT of skull base to assess bony pneumatization near the clivus.
Tailored Approach: Select appropriate surgical route and define extent of bone drilling.
Core Philosophy: Establish a physical multilayer barrier between brain and sinonasal cavity.
Preferred Materials: Autologous vascularized tissues as primary choice, supplemented by synthetic materials as needed.
Postoperative Management: Close observation and early intervention in case of signs of CSF leak.
——————————————————————————————————————————————
Endoscopic Retrograde Catheterization Through the Fourth Ventricle–Aqueduct–Third Ventricle–Lateral Ventricle for Complex Hydrocephalus
ZHU, Weijie – The 960th Hospital of the PLA Joint Logistics Support Force

Case Highlights:
Dr. Zhu presented two complex cases involving low-pressure hydrocephalus, successfully managed through an endoscopic retrograde ventriculostomy and shunt placement via the fourth ventricle to the lateral ventricle, passing through the aqueduct and third ventricle.
Rationale for Retrograde Shunting:
Traditional methods, including aqueductoplasty or supratentorial diversion, were insufficient due to persistent membranous obstructions.
Endoscopy allowed direct visualization and catheter navigation, avoiding blind passage.
Insertion required dilation of the cerebral aqueduct, which can risk brainstem compression if not carefully handled.
Takeaway Message:
While hydrocephalus is common, special subtypes demand nuanced strategies.
Retrograde catheterization is a viable option in select patients, expanding the toolbox for resistant cases.
The technique provoked active debate among the audience, with consensus encouraging long-term follow-up and further outcome studies.
——————————————————————————————————————————————
Neuroendoscopic Treatment of Invasive Pituitary Adenomas
ZHANG, Qingjiu – The Second Hospital of Hebei Medical University

MDT-Centered Approach:
Dr. Zhang emphasized that invasive pituitary tumors require a Multidisciplinary Team (MDT) approach, especially under new policies defining such tumors as “Grade IV surgeries” demanding comprehensive planning.
Three Key MDT Functions:
Personalized Strategy Design – Involving neurosurgeons, endocrinologists, radiologists, and pathologists to evaluate tumor invasiveness, subtype, and patient condition.
Functional Preservation – Prioritize optic chiasm, hypothalamus, and pituitary stalk; avoid visual impairment and endocrine deficiency.
Dynamic Outcome Monitoring – Follow-up with serial MRI, hormone assays, and symptom tracking. Adjust adjuvant treatments like radiotherapy or targeted drugs based on residual disease.
Surgical Challenges & Key Techniques:
Hemostasis: Tumors have rich vascularity, especially near the cavernous sinus; bipolar coagulation, hemostatic agents, and intraoperative hypotension were used to maintain a clear field.
Neuroprotection: Real-time nerve monitoring and navigation helped preserve function and prevent complications like diabetes insipidus.
Skull Base Repair: Employed a multi-layer reconstruction strategy (e.g., synthetic dura + nasoseptal flap + fibrin glue) to seal the sellar floor and prevent CSF leaks.
Endocrine Monitoring: Immediate postoperative corticosteroid replacement in hypophysectomy; urine output and electrolytes monitored for >48 hours post-op.
——————————————————————————————————————————————
Case Discussion Panel
CHEN, Ge – Xuanwu Hospital, Capital Medical University
LOU, Meiqing – Shanghai General Hospital (First People’s Hospital of Shanghai)
GUO, Mian – The Second Affiliated Hospital of Harbin Medical University
Highlighted Topics:
Infection Prevention in Skull Base Surgery:
Mid-case full instrument set replacement.
Culture-driven antibiotic selection.
Clear criteria for escalating antibiotic therapy based on intraoperative contamination.
Postoperative CSF Leak Strategies:
Nasal endoscopic evaluation using ENT surgical setup.
Early repair emphasized.
Smoothing of sellar floor and complete removal of sphenoid mucosa were recommended techniques.
Panel Consensus:
CSF leaks may appear minor but can lead to severe complications including meningitis and prolonged hospitalization. The emphasis remains on strict prevention, early detection, and decisive repair.
——————————————————————————————————————————————
4.Exhibition Highlights: Advancing Neurosurgical Solutions

In parallel with the scientific sessions, Medprin’s exhibition booth became a focal point for attendees, presenting an integrated portfolio under the theme of Neurosurgery and Advanced Surgical Solutions.
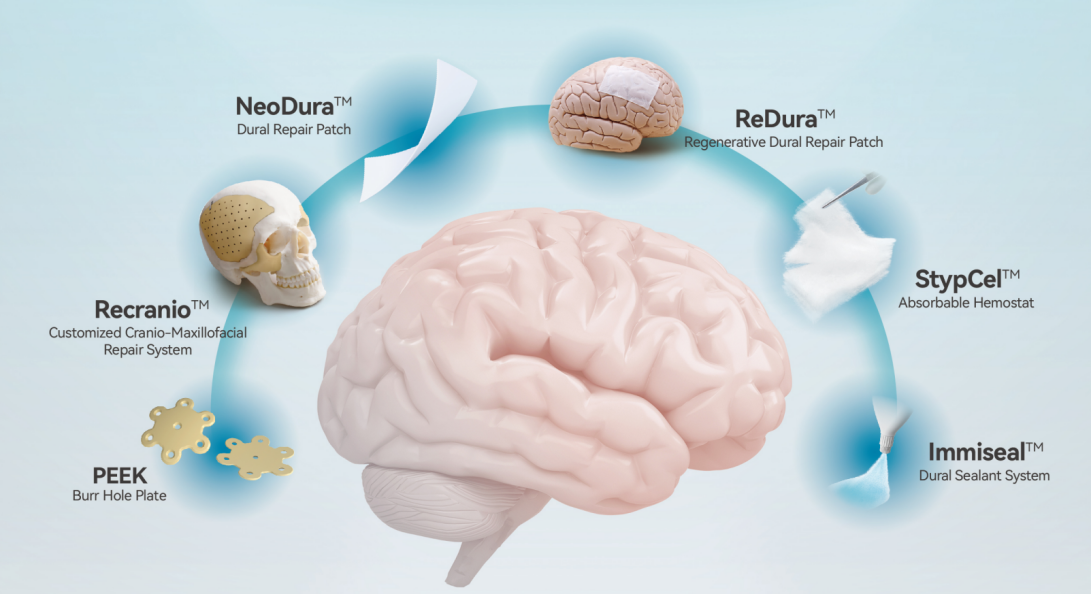
Through immersive demonstrations and hands-on interaction, the booth illustrated how Medprin integrates additive manufacturing technology and advanced biomaterials into its product lines, delivering high-quality, innovative solutions that empower neurosurgeons worldwide.

The exhibition area attracted a large number of domestic and international neurosurgeons, sparking in-depth conversations on clinical applications and future collaborations.
5.Closing Remarks: Sharing Innovations, Inspiring Global Practice
This year’s sessions demonstrated not only the technical depth of Chinese neurosurgical practice but also the openness to share experience with the global community. From meticulous skull base reconstruction strategies aimed at preventing cerebrospinal fluid leakage, to innovative endoscopic techniques for complex hydrocephalus, to multidisciplinary approaches in managing invasive pituitary adenomas, each case offered practical insights that transcend geographic boundaries.
The recurring theme was clear: precise preoperative planning, strategic material selection, and timely postoperative intervention form the cornerstone of successful neurosurgical outcomes. The preventive philosophy—anticipating complications such as CSF leakage before they occur—was repeatedly emphasized as the most effective way to safeguard patients.
By openly discussing operative techniques, complication management, and device innovations, Chinese neurosurgeons are contributing valuable knowledge to a shared global mission: improving surgical safety, expanding treatment possibilities, and enhancing patient quality of life.
As the conference concluded, it was evident that these lessons, rooted in rigorous clinical practice and bolstered by advanced technology, will continue to inform and inspire neurosurgical teams worldwide.







